
Team Leaders
- Dr Nicola Simmonds, Consultant Gastroenterologist
Luton and Dunstable Hospital. E-mail: nicola.simmonds.ldh.nhs.uk
Team Members
- Nicola Simmonds, Consultant Gastroenterologist
- Hazel Rollins, Nutrition Nurse Specialist
- April Smith, Chief Dietitian
- Sue Batty, Catering Services Manager
- Jacqui Arnold, Nutrition Research Nurse
- Alison Balman, Senior Dietitian
The team could not have done this without the great support from the Trust Chief Executive, Stephen Ramsden and the Trust Chariman, Eric Fountain.
What was the problem you were trying to address?
Our Trust had taken the decision in 1996 to introduce a soup and sandwich evening meal. There was concern from the dietitians and nutrition nurse specialist that this would have a detrimental effect on patients’ food intake. This led to a weighed food intake demonstrating that no patient met their recommended daily energy and only 2/20 patients met their protein requirements. A patient satisfaction survey had shown that 21% of patients did not enjoy the evening meal and there had been a 27% increase in dietetic referrals over a year and a 19% increase in the monthly expenditure on oral nutritional supplements.
In 1998 we received charitable funds for our “Eating Matters” project. This was a broad ranging project attempting to address every stage of nutritional care from nutritional screening, food availability and service, staffing and monitoring.
How did you create your project plan?
We started by identifying all the stakeholders in the delivery of nutritional care to patients and by creating a process map of all the various steps involved. Meetings were help to ensure all the following staff groups were included in the consultation exercise:
Senior nurses, ward sisters and nutrition link nurses
- Dietitians
- Caterers
- Therapists
- Fire Officer
- Nutrition Steering Committee members
- Medical staff
The members of the project team met on a weekly basis to discuss progress and drive further actions. The project would not have been possible without the nutrition research nurse who was responsible for the day to day data collection and coordination with the other stakeholders to purchase the new equipment, appoint and train the additional staff and liaise with the dietitians and catering department over the improvements in food provision.

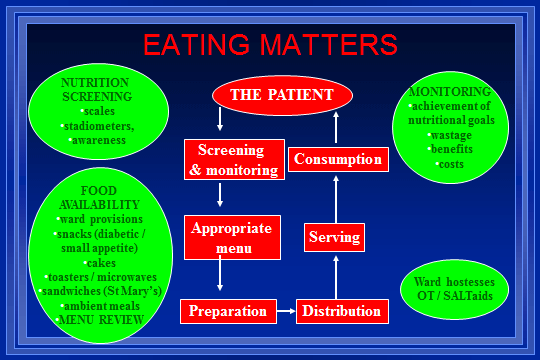
Key Actions
- Provide additional equipment (scales, stadiometers, toasters, microwave ovens on the wards, specialist crockery and cutlery)
- Provide additional food (diabetic snacks, snacks for small appetites, cakes with afternoon tea, sandwiches for the Day Hospital, ward provisions)
- Review the patient menu (Improved range and supply of ward provisions, re-introduction of a cooked evening meal, improved ethnic meals, changed sandwich supplier, porridge made with milk not water, improved choices on menu, patient feedback encouraged)
- Employ new staff (nutrition research nurse, 2 ward hostesses)
- Monitor outcomes (nutrition risk screening audit, weight change study, patient satisfaction survey, weighed food intake study, food wastage, dietetic contact episodes, oral nutritional supplement use, observational audit, length of hospital stay, toaster fires)
Main Outcomes
- Improved patient screening (recording of weight increased from 57% to 91%, height from 6% to 61% and BMI from 11% to 33%)
- Reduced plate waste
- Reduced tray waste on wards with ward hostesses (by 3-8%). Other wards showed an increase in tray waste over the same period, particularly in surgery where levels ranged from 24-33% wasted).
- Greater food availability on wards with ward hostesses
- Specialist feeding equipment makes one quarter of those using it independent in feeding
- Far fewer toaster fires (from 29 to 2 per year) – ensuring toast is readily available on all the wards
- Patient satisfaction improved, with the numbers rating their meals as good or very good increasing from 47% to 63% and those rating their meals as poor or very poor decreasing from 19% to 6%
- Increased numbers of patients meeting >95% of their energy (from7% to 47%) and protein requirements (from 11% to 52%)
- Patients lose less weight (in Medicine the percentage of patients losing weight during their hospital stay reduced from 22% to 15%)
- Reduced supplement use (from a peak of 3500 units per month to 1500 units per month)
- Increased dietetic referrals (the number of dietetic contacts increased from 6521 to 8801)
- Reduced average length of stay in Medicine from 4.8 days in 1998 to 4.3 days in 2000
How are you going to maintain the improvement?
This proved to be the greatest challenge. We were able to translate much of the work we had already done into implementing the Better Hospital Food programme. However, catering yet again became the target for savings and we struggled to maintain the crucial working relationship with the catering department that is essential to ensuring adequate food availability on the ward. We were also unable to extend the ward hostess programme, despite the evidence of cost savings in terms of reduced waste.
We concluded that in the days of competing priorities for finance, the priority was to ensure that nutrition was mandated as part of commissioning, with financial penalties for failure to achieve targets. We ensured that our Trust was one of the first wave Trusts taking part in the Patient Safety Express programme and that this was supported at a senior level. Nutritional care on the Care of the Elderly wards is now also a CQUIN and we are pleased to report that the staff on the ground remain passionate about good nutritional care.
Tips for others planning similar projects
- Identify all your stakeholders
- Engage senior management
- Be realistic about the amount of time it will take
- Lobby hard for sufficient resources
- Ensure that you foster a great relationship between the catering department and the wards
- Develop a robust communications plan
Top Quotes




